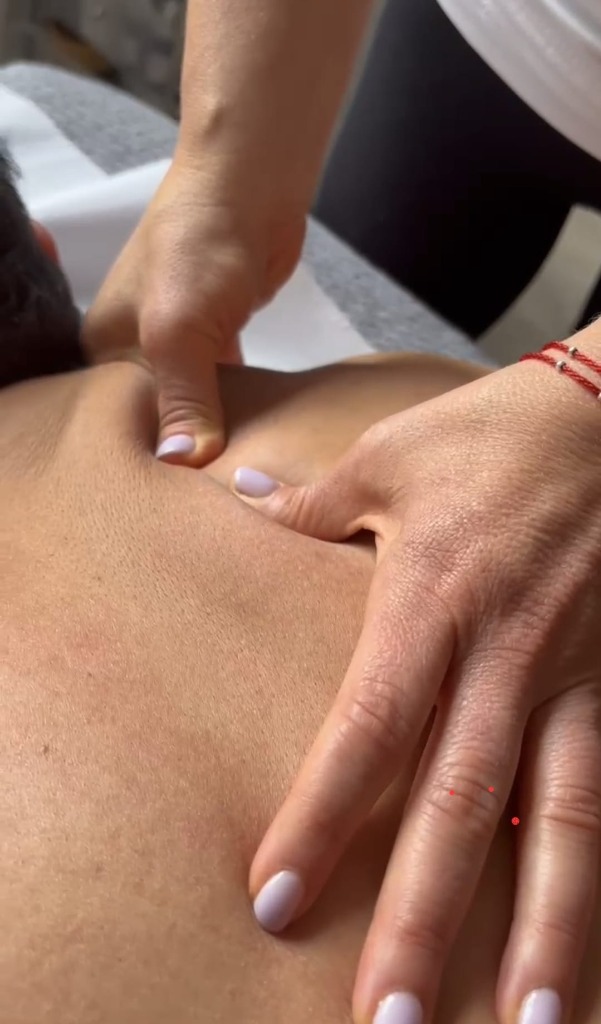
What Is a Muscle Knot, Really?
The term "muscle knot" is universally understood but scientifically misleading. What you feel as a hard, painful lump in your muscle is actually a myofascial trigger point — a localised area of hypercontracted sarcomeres (the smallest contractile units of muscle fibre) embedded within a taut band of skeletal muscle.
The landmark research by Travell & Simons, published in their Myofascial Pain and Dysfunction textbook (now in its third edition), established that trigger points are not inflammation, not scar tissue, and not muscle spasm in the traditional sense. They are a self-sustaining neurochemical event at the motor end plate — the junction where the nerve tells the muscle to contract.
The Integrated Trigger Point Hypothesis
The currently accepted scientific model, known as the Integrated Trigger Point Hypothesis (Gerwin, Dommerholt & Shah, 2004), explains the mechanism in five steps:
- Motor end plate dysfunction — excessive acetylcholine release at the neuromuscular junction causes a sustained localised contraction
- Sarcomere shortening — the affected sarcomeres lock in a contracted state, forming the palpable "knot"
- Local ischaemia — the contracted tissue compresses nearby capillaries, reducing blood flow and oxygen delivery
- Energy crisis — without adequate oxygen, the muscle cannot produce enough ATP to release the contraction (relaxation is an active process that requires energy)
- Sensitising substances accumulate — substance P, calcitonin gene-related peptide (CGRP), bradykinin and other inflammatory mediators collect in the ischaemic zone, activating nociceptors (pain receptors) and causing both local and referred pain
A groundbreaking study by Shah et al. (2008) in the Journal of Bodywork and Movement Therapies confirmed this model by inserting microdialysis needles directly into active trigger points. They found concentrations of inflammatory mediators up to 10 times higher than in normal tissue.
Why Do Trigger Points Form?
- Sustained postures — holding any muscle in a shortened or lengthened position for hours (desk work, driving) creates the conditions for end-plate dysfunction
- Repetitive motion — overloading the same motor units without adequate recovery
- Acute overload — a sudden, heavy lift or awkward movement that exceeds the muscle's capacity
- Emotional stress — limbic system activation increases baseline motor unit firing, particularly in the upper trapezius, temporalis and masseter
- Sleep deprivation — reduced growth hormone output impairs the nocturnal tissue repair that would normally resolve early-stage trigger points
How Deep Tissue Massage Resolves Trigger Points
1. Ischaemic Compression
Sustained thumb or elbow pressure on the trigger point initially increases ischaemia — which sounds counterintuitive. However, upon release, a reactive hyperaemia occurs: blood rushes into the previously compressed tissue, delivering oxygen, ATP and nutrients while flushing out the accumulated sensitising substances. Research in Archives of Physical Medicine and Rehabilitation (2013) showed that a single 90-second compression reduced trigger point sensitivity by 37%.
2. Mechanical Disruption of Sarcomere Contraction
Deep sustained pressure physically separates the locked sarcomeres, breaking the contraction cycle. The therapist works along the direction of the muscle fibres, systematically "ironing out" the taut band from origin to insertion.
3. Neurological Reset
Trigger point release activates the Golgi tendon organ — a proprioceptive receptor that monitors muscle tension. When stimulated by sustained pressure, it sends an inhibitory signal via the spinal cord that forces the muscle to relax. This neurological reset breaks the self-sustaining contraction cycle at the motor end plate.
4. Fascial Sliding Restoration
Trigger points create fascial adhesions between the muscle and its surrounding connective tissue sheath. Deep tissue strokes restore the gliding between these layers, reducing the mechanical restriction that perpetuates the trigger point.
Common Trigger Point Referral Patterns
One of the most clinically important aspects of trigger points is that they refer pain to distant areas. Understanding these patterns is essential for effective treatment:
- Upper trapezius → pain at the temple, behind the eye, angle of the jaw
- Infraspinatus → deep shoulder pain, pain down the outer arm to the hand
- Quadratus lumborum → pain in the hip, sacroiliac joint, lower buttock
- Gluteus minimus → pain down the lateral leg, mimicking sciatica
- Soleus → heel pain and plantar fascia-like symptoms
This is why treating only the site of pain often fails. At Mayfair Massage & Therapy, we trace the referral pattern back to its source and treat the trigger point directly — which is why clients often say "That's exactly my pain!" when the correct point is found.
"A trigger point in your infraspinatus can produce deep shoulder pain that mimics a rotator cuff tear. A trigger point in your soleus can mimic plantar fasciitis. The skill lies in knowing where to look — not just where it hurts."
— Concetta, Lead Therapist